Regenerative medicine is a relatively recent development. Throughout history, there have been longstanding speculations about the potential for natural or medical regeneration of our bodies. However, it wasn’t until the 20th century that significant scientific strides were made, leading to the establishment of the field. If the term “regenerative medicine” is unfamiliar to you, you might be more familiar with the term “stem cell research.” At its core, regenerative medicine operates on the fundamental principle that our cells possess an inherent ability to regenerate. By utilizing a combination of therapies, treatments, and surgical procedures, we have the potential to enhance and optimize our body’s natural healing capabilities.
As we embark on a journey through the fascinating realm of Regenerative Medicine in 2024, this blog promises to be your destination for the most current and relevant information. We’ll demystify the science behind regenerative medicine and explore the diverse applications of this innovative field. We’ll also delve into the transformative world of regenerative medicine, addressing the frequently asked question: is regenerative medicine legit? Whether you’re a healthcare professional or a patient interested in revolutionary treatments, this blog is your compass to navigate the evolving landscape of regenerative medicine in 2024.
What is Regenerative Medicine?
Regenerative medicine is a multidisciplinary field of medical science that focuses on the development of therapies and treatments aimed at restoring, repairing, or replacing damaged or diseased tissues and organs in the human body. The primary goal of regenerative medicine is to harness the body’s natural ability to heal itself and promote tissue regeneration.
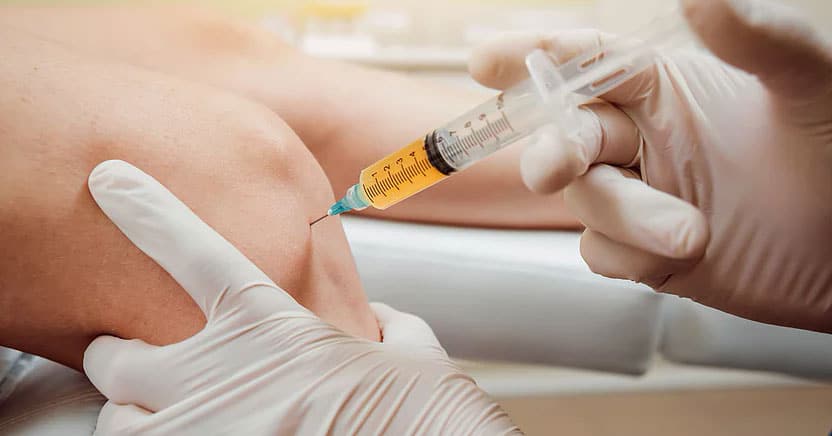
Types of Regenerative Medicine
There are several key approaches within regenerative medicine, each with its own unique methods and applications.
- Cellular Therapies: Cellular therapies harness the power of the body’s own cells to promote healing. This category includes treatments like stem cell therapy and platelet-rich plasma (PRP) therapy.
- Gene Therapy: Gene therapy is a revolutionary approach that involves modifying a patient’s genes to treat or prevent disease.
- CRISPR-Cas9 Technology: CRISPR-Cas9 is a powerful gene-editing tool that can be used to target and modify specific genes. This technology has the potential to correct genetic defects that underlie a wide range of diseases.
- Gene Editing for Regenerative Purposes: gene editing can be used to enhance the regenerative capacity of cells or tissues. For example, researchers are exploring ways to edit genes in stem cells to make them more effective at regenerating damaged tissues.
- Small Molecule Therapies: Small molecules are compounds that can influence cellular processes and signaling pathways. These molecules can be used to stimulate tissue regeneration and repair.
- Growth Factors and Signaling Molecules: Growth factors are proteins that play a key role in cell growth, differentiation, and tissue repair. By administering specific growth factors, researchers and clinicians can promote tissue regeneration in targeted areas.
- Pharmaceutical Interventions: Pharmaceutical drugs can be used to modulate cellular processes involved in tissue repair. These drugs may enhance the body’s natural regenerative responses or suppress harmful inflammatory processes.
What Can Regenerative Medicine Treat?
Regenerative medicine has the potential to address a wide range of conditions. It offers hope to individuals who may have previously faced limited treatment options. Let’s explore some of the key medical areas where regenerative medicine is making significant strides:
Orthopedic Conditions
- Osteoarthritis: Osteoarthritis is a degenerative joint condition characterized by the breakdown of cartilage in the joints. Regenerative therapies, such as stem cell therapy and PRP, have shown promise in promoting cartilage repair and reducing pain and inflammation.
- Tendon Injuries: Conditions like tendinitis and rotator cuff injuries can be challenging to treat. Cellular therapies can target damaged tendons and promote tissue regeneration, potentially improving function and reducing pain.
- Dermatology:
- Hair Loss: PRP is used in some cases to promote hair growth in individuals experiencing certain types of hair loss, such as androgenetic alopecia.
- Facial Rejuvenation: PRP is sometimes employed in cosmetic procedures, such as the “vampire facelift,” to enhance skin texture and promote collagen production.
- Dentistry:
- Dental Implants: PRP may be used to accelerate the healing process and enhance bone regeneration after dental implant surgery.
- Oral Surgery: PRP is explored in procedures such as tooth extractions and jaw surgeries to facilitate healing.
- Sports Medicine:
- Muscle Injuries: PRP has been investigated for its potential in treating muscle injuries, such as strains or tears.
- Chronic Wounds:
- Non-healing Wounds: PRP has been studied as a potential therapy for chronic, non-healing wounds, such as diabetic ulcers.

Global Impact and Access of Regenerative Medicine
One of the most profound attributes of regenerative medicine is its potential to bridge healthcare disparities on a global scale. Researchers and organizations are passionately committed to ensuring that regenerative treatments are accessible to all, transcending geographical and socioeconomic barriers. This mission encompasses multifaceted strategies, including making treatments more cost-effective, optimizing distribution networks, and providing essential training to healthcare professionals in underserved regions.
Global initiatives are emerging as dynamic platforms for knowledge sharing and capacity building. Their overarching objective is crystal clear: to democratize access to healthcare solutions, ensuring that the benefits of regenerative medicine extend to every corner of the world. It’s about leveling the healthcare playing field, making sure that everyone has an equal opportunity to enjoy better health.
What Is Regenerative Medicine Used For?
Regenerative medicine is incredibly versatile, offering innovative solutions to a wide range of medical conditions and chronic diseases. From orthopedics to cardiology, it is transforming the treatment landscape by addressing previously unmet needs.
Orthopedics
In the field of orthopedics, regenerative medicine is playing a pivotal role in treating musculoskeletal conditions. Common applications include the use of platelet-rich plasma (PRP) and stem cell therapies for conditions such as osteoarthritis, tendon injuries, and ligament damage. By harnessing the body’s natural healing processes, these treatments offer the potential for pain relief, improved mobility, and delayed joint replacements.
Cardiology
Regenerative medicine is making significant strides in cardiology. It is exploring novel approaches to repair damaged heart tissue, especially after myocardial infarctions (heart attacks). Researchers are investigating the use of stem cells and growth factors to stimulate cardiac tissue regeneration and improve heart function. This breakthrough could lead to enhanced recovery and reduced risks for heart failure patients.
Neurology
Neurological disorders such as Parkinson’s disease, Alzheimer’s disease, and spinal cord injuries have traditionally been challenging to treat. Regenerative medicine is opening up new avenues of hope. Stem cell therapies are being investigated to replace damaged neural cells and enhance the function of the central nervous system. While these treatments are still in the experimental phase, they hold the promise of substantial improvements in the quality of life for patients with these debilitating conditions.
Dermatology
The field of dermatology benefits from regenerative medicine through innovative skin tissue engineering. Patients with extensive burns, chronic wounds, or skin defects due to injury or disease can experience remarkable improvements. Bioengineered skin grafts, created from a patient’s own cells, can be used to repair damaged areas, reducing scarring and enhancing the natural healing process.
Gastroenterology
Regenerative medicine has also ventured into gastroenterology. Patients with conditions such as Crohn’s disease or ulcerative colitis may benefit from stem cell therapies to repair damaged intestinal tissue. These treatments aim to reduce inflammation, promote tissue healing, and alleviate symptoms, offering a ray of hope for those suffering from chronic digestive disorders.
Urology
Regenerative medicine holds potential for patients with urological issues, such as erectile dysfunction or urinary incontinence. Stem cell therapies and tissue engineering techniques are being explored to rejuvenate and repair damaged tissues in the genitourinary system, offering new solutions for individuals seeking to regain normal function and improve their quality of life.
Ophthalmology
Eye disorders and vision loss have been challenging to address effectively. However, regenerative medicine is breaking new ground in ophthalmology. Researchers are investigating stem cell-based approaches to repair damaged retinal tissue, potentially restoring vision in conditions like macular degeneration and retinitis pigmentosa.
In 2024, regenerative medicine is continuing to expand its scope and reach, providing hope for patients with a wide range of medical conditions. The potential applications of regenerative therapies are only limited by the extent of ongoing research and clinical trials, and as the field evolves, we can expect even more breakthroughs that will positively impact the lives of countless individuals.
Is Regenerative Medicine Legit?
Regenerative medicine is not without controversy, and many have questioned its legitimacy. However, it’s important to note that this field is heavily regulated and has a substantial body of scientific evidence supporting its effectiveness. The legitimacy of regenerative medicine is underpinned by rigorous research, clinical trials, and regulatory oversight. With that said their are doctors that utilize forms of regenerative medicine that have not been approved and so you should always do your due diligence to find a provider who has been specially trained and has the proper qualifications.
In fact, the scientific community has been dedicated to the validation of regenerative therapies through comprehensive research and stringent clinical trials. These trials involve large-scale studies with diverse patient populations, ensuring that treatments are thoroughly evaluated for both safety and efficacy. Moreover, regulatory bodies, such as the FDA in the United States, closely oversee the development and approval of regenerative treatments to guarantee their adherence to the highest standards of patient safety.
The robust foundation of scientific evidence and regulatory scrutiny gives patients and healthcare professionals confidence in the legitimacy of regenerative medicine. It is a field that has evolved and matured, leaving little room for unfounded skepticism. Today, regenerative medicine is emerging in clin
The Biggest Problem with Regenerative Medicine
While regenerative medicine holds immense promise, it faces ethical and regulatory challenges. Ensuring that treatments are safe, effective, and well-regulated is a critical concern. In 2024, these challenges have prompted a concerted effort by regulatory bodies and the scientific community to establish clear guidelines and ethical frameworks for the responsible practice of regenerative medicine.
One of the significant challenges in regenerative medicine is defining and maintaining ethical standards, especially regarding the use of certain cell types like embryonic stem cells. Researchers and policymakers have worked diligently to strike a balance between scientific progress and ethical considerations. This ongoing dialogue seeks to address concerns and establish protocols that respect the moral boundaries of research and treatment in regenerative medicine.
Moreover, ensuring that regenerative treatments are administered by qualified healthcare professionals in accredited facilities is another crucial aspect of regulation. This oversight helps prevent the proliferation of unregulated clinics offering unproven treatments, thereby safeguarding patients from potential risks and fraudulent practices.
As the field matures, the scientific community continues to collaborate with ethical and regulatory bodies to navigate these challenges and maintain the highest standards of safety and effectiveness in regenerative medicine.
Does Regenerative Medicine Really Work?
Regenerative medicine is a rapidly evolving field that aims to restore or replace damaged tissues and organs using various approaches, including stem cell therapy, tissue engineering, and gene therapy. Whether regenerative medicine “really works” depends on the specific application, the state of the science at the time, and the definition of success.
Regenerative medicine has shown promise and demonstrated success in several areas, and I can provide some examples:
- Stem Cell Therapies: Stem cells have the potential to develop into different cell types, making them a valuable tool in regenerative medicine. Stem cell-based treatments have been successful in bone marrow transplants to treat conditions like leukemia and certain blood disorders. There are also ongoing clinical trials for various other applications, including heart disease, neurodegenerative disorders, and diabetes.
- Tissue Engineering: Scientists have made progress in growing replacement tissues and organs in the lab. For instance, skin grafts, cartilage, and bladder tissue have been successfully engineered and used in patients. More complex organs, like kidneys and livers, are still in the experimental stages, but progress is being made.
- Gene Therapy: Gene therapy has shown success in treating certain genetic disorders. For example, treatments for conditions like spinal muscular atrophy and certain types of inherited blindness have been approved by regulatory agencies.
- Cartilage Repair: Regenerative medicine techniques, such as autologous chondrocyte implantation (ACI) and matrix-induced autologous chondrocyte implantation (MACI), have been used to repair damaged cartilage in the knee. Stem cell therapy also assists with the regrowth of cartilage in knees and other joints.
- Burn Wound Healing: Stem cell-based therapies and tissue-engineered skin have been used to treat burn patients and promote skin regeneration.
While there are many successes, it’s important to note that regenerative medicine is still an emerging field, and not all applications have achieved widespread clinical use or regulatory approval. The outcomes of treatments can vary depending on factors like the type of injury or disease, the patient’s specific condition, and the treatment protocols.
Additionally, regenerative medicine is an area of active research and development, so what might not be considered a “working” treatment today could become a reality in the near future as new advancements are made.
Diseases Treated with Regenerative Medicine
Regenerative medicine has the potential to treat a wide range of medical conditions, from degenerative joint diseases to heart failure. Explore how it’s being applied in various fields. In 2024, the list of diseases treated with regenerative medicine continues to expand. Conditions such as osteoarthritis, diabetes, and even neurological disorders like Alzheimer’s disease are being explored for regenerative interventions. The most common diseases in 2024 treated by regenerative medicine are degenerative joint diseases.
The expanding scope of diseases treated with regenerative medicine is a testament to the field’s versatility and potential. Regenerative therapies are not limited to a specific medical domain; they hold promise across a broad spectrum of conditions. Researchers and clinicians are continually exploring new applications and pushing the boundaries of what is possible.
For instance, in the field of neurology, regenerative medicine offers hope to patients with previously untreatable conditions, potentially improving their quality of life. The ongoing efforts to expand the range of treatable diseases are a reflection of the commitment to advancing healthcare through regenerative approaches.
Disadvantages of Regenerative Medicine
While regenerative medicine offers significant advantages, it also comes with its share of limitations and challenges. In 2024, some of the common disadvantages include the high cost of treatments, the need for specialized facilities, and the complexity of some regenerative procedures.
High Cost of Treatments
The high cost of regenerative treatments can pose a barrier to access for some patients. As mentioned later in the blog, regenerative medicine therapies can cost from hundreds, to tens of thousands of dollars depending on the treatment. The development and production of regenerative therapies, especially those involving tissue engineering or personalized medicine, can be resource-intensive. However, it’s worth noting that ongoing research and technological advancements are gradually reducing the cost of these treatments, making them more accessible to a broader range of patients.
Lack of Trained Facilities
Additionally, specialized facilities and expertise are essential for the successful administration of regenerative therapies. Not all healthcare institutions may have the necessary infrastructure or trained personnel, which can limit the availability of these treatments in some regions. Efforts are being made to expand access by training healthcare professionals and creating partnerships between facilities to share expertise.
The complexity of some regenerative procedures, such as growing personalized organs or navigating the intricacies of stem cell therapy, can also present challenges. However, these challenges are being met with ongoing research and collaboration to streamline and simplify regenerative treatments for the benefit of patients.
Who Is a Good Candidate for Regenerative Medicine?
A good candidate for regenerative medicine regarding joint pain would have some cartilage and tissue remaining between bones.
Personalized medicine is a key aspect of regenerative medicine, ensuring that treatments are tailored to the specific needs of individual patients. Genetic testing and predictive analytics are increasingly used to identify candidates who are likely to benefit the most from regenerative therapies. This personalized approach enhances treatment outcomes and minimizes potential risks.
Patients with conditions that have not responded to traditional treatments or those seeking alternatives to invasive surgeries often find regenerative medicine to be a viable option. Surgery is considered to be the last straw for certain conditions. Regenerative medicine can be more affordable, as well as have a more positive outcome than surgery. It is highly emphasized that people considering surgery can be a great candidate for regenerative medicine.
By identifying suitable candidates through personalized medicine, healthcare providers can offer the most appropriate regenerative treatments while maximizing the chances of success. In 2024, the integration of advanced diagnostic tools and predictive technologies is fine-tuning the selection of candidates for regenerative therapies, ultimately leading to more precise and effective treatments.
Success Rate of Regenerative Therapy
Success rates in regenerative medicine treatments can vary. Factors such as patient age, overall health, and the specific condition being treated can influence outcomes. In 2024, success rates continue to improve as more data is collected, and treatments are refined. For example, in orthopedic regenerative procedures, success rates are notably high, with many patients experiencing significant pain relief and improved mobility.
“Once entering Phase 1, rare disease durable gene therapies are two to three-and-a-half times more likely to gain FDA approval compared to the average drug across all modalities. In comparing success rates by phase of clinical development, gene therapies outperform average drugs at every step. The analysis shows that the average rare disease gene therapy has a 28% chance of receiving FDA approval once it enters Phase 1.”
Compared to average drugs included in the BIO Report, orphan gene therapies had:
• 48% higher success rate in Phase 1 clinical trials
• 65% higher success rate in Phase 2 clinical trials
• 30% higher success rate in Phase 3 clinical trials
• 10% higher success rate in completing a New Drug Application (NDA) or Biologics License Application (BLA)
In orthopedic regenerative procedures like PRP therapy or stem cell treatments for joint issues, success rates have been particularly promising. Many patients have reported significant pain relief, improved mobility, and a better quality of life following these treatments. This positive trend is attributed to the ongoing refinement of regenerative protocols and techniques, which enhances their effectiveness.
Continued collaboration between healthcare professionals and researchers, along with a dedication to evidence-based practices, ensures that regenerative therapies continue to offer higher success rates and better outcomes for patients.
Why Is Regenerative Medicine Controversial?
Ethical concerns and public misconceptions have led to controversy surrounding regenerative medicine. It is essential to understand and address these issues. In 2024, the controversy around regenerative medicine primarily revolves around the ethical use of embryonic stem cells and concerns about unregulated clinics offering unproven treatments. Public education and responsible research practices are essential for addressing these controversies.
Ethical Considerations and Regulations:
The controversy surrounding regenerative medicine often centers on two main issues: ethical considerations related to the use of embryonic stem cells and concerns about the proliferation of unregulated clinics offering unproven treatments.
Embryonic stem cells have immense regenerative potential, but their use raises ethical questions due to the source of these cells. The ongoing dialogue within the scientific and ethical communities aims to establish guidelines and principles that strike a balance between scientific progress and moral considerations. Researchers are exploring alternative sources of stem cells, such as induced pluripotent stem cells, to address these concerns.
The rise of unregulated clinics offering unproven regenerative treatments is a cause for concern. It highlights the need for robust regulatory oversight and public education. In response, regulatory bodies and healthcare professionals are working together to develop clear guidelines and ensure the responsible practice of regenerative medicine. Public education campaigns aim to inform patients about the importance of seeking treatments from accredited, reputable sources.
The resolution of these controversies requires open dialogue, ethical guidelines, and a commitment to responsible research and treatment practices in the field of regenerative medicine. They are many different sources for stem cell therapy that one can choose from.
Recovery Time for Regenerative Medicine
Post-treatment recovery times differ depending on the type of regenerative therapy. Understand what to expect during the recovery process. In 2024, many regenerative procedures offer shorter recovery times compared to traditional surgical interventions. For instance, platelet-rich plasma (PRP) therapy is known for its relatively short recovery periods. Patients undergoing PRP therapy for musculoskeletal injuries often experience minimal downtime and can return to their daily activities within a few days. This rapid recovery is a testament to the non-invasive and minimally disruptive nature of many regenerative treatments.
The recovery time for stem cell therapy can vary significantly depending on several factors, including the type of stem cell therapy, the specific condition being treated, and individual patient factors. In general, here’s what you can expect:
- Minimal Recovery (Same Day or Within a Few Days):
- Some stem cell treatments, such as those involving adipose-derived stem cells (from fat tissue) or bone marrow-derived stem cells, may have minimal recovery time. Patients might experience mild soreness at the site of stem cell extraction (e.g., the hip for bone marrow) but can typically resume their daily activities shortly after the procedure.
- Short-Term Recovery (A Few Days to a Few Weeks):
- For certain conditions or treatment methods, patients might experience a short-term recovery period. This could involve some discomfort or swelling at the injection site. Activities may be limited for a few days to a few weeks, but most individuals can return to their normal routines relatively quickly.
- Longer Recovery (Several Weeks to Months):
- In more complex cases or when stem cell therapy is combined with other medical interventions, such as surgery, the recovery time may be more extended. Some patients may require several weeks to months to fully recover and experience the full benefits of the therapy.
It’s essential to note that the specific recovery time can vary based on the individual’s overall health, the condition being treated, and the chosen therapy approach. Patients should always follow their healthcare provider’s post-treatment instructions, including any restrictions on physical activities, to optimize their recovery and ensure the best possible outcomes.

How much does Stem Cell Therapy cost?
Stem cell therapy, a cutting-edge field in medical science, offers promising treatment options for a wide range of medical conditions. However, cost is a critical consideration for many patients when exploring this innovative avenue of regenerative medicine. The price of stem cell treatments in 2024 can vary significantly, making it essential for individuals to understand the factors that influence these costs and whether insurance coverage is a possibility. The price range for stem cell therapy typically costs between $3,500-$50,000.
Why is There a Price Range?
The specific cost of stem cell therapy is influenced by several key factors, starting with the type of treatment required. Conditions can vary in complexity, and treatments for orthopedic issues like joint pain or osteoarthritis may be more cost-effective than therapies for more intricate ailments such as neurological disorders or autoimmune diseases. The geographical location of the treatment facility is another significant factor. Medical services in urban centers and developed countries typically come with a higher price tag than in rural or developing regions.
Moreover, the reputation and expertise of the clinic and its medical professionals play a crucial role in cost determination. Renowned clinics with a history of successful outcomes and experienced staff may charge a premium for their services, often reassuring patients with the promise of quality care. Additionally, the source and processing of stem cells used in therapy can affect costs, as different types of stem cells, such as embryonic, adult, or induced pluripotent stem cells, each come with varying production expenses.
The number of therapy sessions required also contributes to the total cost, as some conditions demand multiple treatments for optimal results. Additionally, the delivery method of the stem cell therapy can impact expenses. More invasive methods, like surgical procedures, generally accumulate higher costs due to their complexity. Beyond the treatment itself, patients should consider other services, including pre-treatment evaluations, post-treatment follow-ups, and any necessary rehabilitation, which can add to the overall expense.
Will My Treatment be Covered By Insurance?
When it comes to insurance coverage, many traditional health insurance plans may not cover stem cell therapy. This is particularly common because these therapies are considered experimental or not widely accepted within the medical community. However, with the insurance landscape is evolving, with some providers starting to offer partial coverage for specific stem cell treatments.
To make stem cell therapy more accessible to patients, some healthcare providers and clinics offer financing options. These may include payment plans, medical loans, or partnerships with financing institutions. These options allow patients to spread the cost of treatment over time, reducing the upfront financial burden. As a result, it’s vital for patients to inquire about these possibilities and carefully consider their financial resources when exploring stem cell therapy.
Conclusion
In the world of medicine, regenerative therapies are rewriting the rules. This ultimate guide has provided you with a comprehensive overview of regenerative medicine. From its inception to its current state in 2024, we encourage you to explore the possibilities it offers. Consult with healthcare professionals to stay updated on the latest developments in this dynamic and transformative field.
The impact factors of regenerative medicine, its various types, the conditions it can treat, eligibility criteria, and efficacy all contribute to a rapidly evolving landscape. With ongoing research, collaboration, and innovation, regenerative medicine continues to hold the promise of improving the lives of countless individuals worldwide. By staying informed and engaging, you can be part of this transformative journey towards a healthier future.
________________________________________________________________________________________________________________
References
DiMasi, J.A., Feldman, L., Seckler, A. and Wilson, A., 2010.
Trends in risks associated with new drug development: success rates for investigational drugs. Clinical Pharmacology &
Therapeutics, 87(3), pp.272-277. https://ascpt.onlinelibrary.
wiley.com/doi/abs/10.1038/clpt.2009.295
Petrosyan A, Martins PN, Solez K, Uygun BE, Gorantla VS, Orlando G. Regenerative medicine applications: An overview of clinical trials. Front Bioeng Biotechnol. 2022 Nov 25;10:942750. doi: 10.3389/fbioe.2022.942750. PMID: 36507264; PMCID: PMC9732032.
Sebbagh P, Cannone A, Gremion G, Gremeaux V, Raffoul W, Hirt-Burri N, Michetti M, Abdel-Sayed P, Laurent A, Wardé N, Applegate LA. Current Status of PRP Manufacturing Requirements & European Regulatory Frameworks: Practical Tools for the Appropriate Implementation of PRP Therapies in Musculoskeletal Regenerative Medicine. Bioengineering (Basel). 2023 Feb 24;10(3):292. doi: 10.3390/bioengineering10030292. PMID: 36978683; PMCID: PMC10044789.
Wong, C.H., Siah, K.W. and Lo, A.W., 2019. Estimation of
clinical trial success rates and related parameters. Biostatistics,
20(2), pp.273-286. https://academic.oup.com/biostatistics/
article/20/2/273/4817524
Wyles SP, Monie DD, Paradise CR, Meyer FB, Hayden RE, Terzic A. Emerging workforce readiness in regenerative healthcare. Regen Med. 2021 Mar;16(3):197-206. doi: 10.2217/rme-2020-0137. Epub 2021 Feb 24. PMID: 33622054; PMCID: PMC8656339.