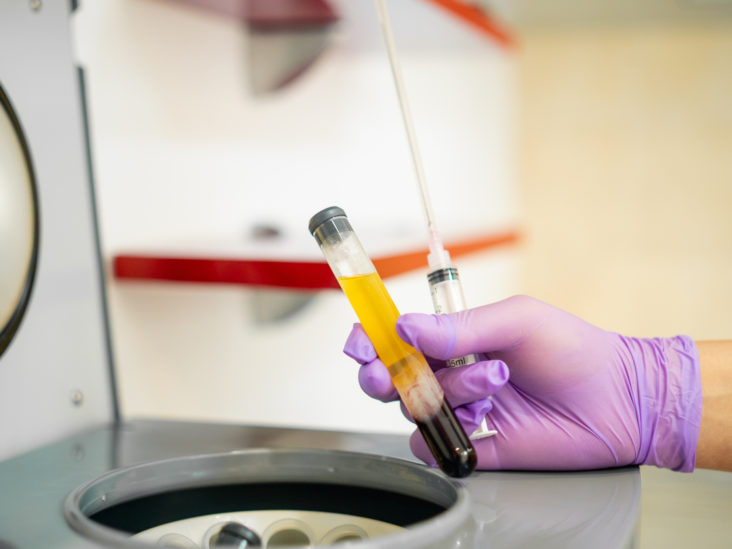
Platelet-rich Plasma (PRP Injections)
Platelet-rich plasma (PRP) therapy is employed to expedite the recovery process for damaged tendons, ligaments, muscles, and joints. This treatment entails the administration of injections containing a concentrated amount of a patient’s own platelets. Through the utilization of PRP injections, we harness the innate healing capabilities of each patient to enhance their musculoskeletal conditions. PRP therapy is particularly effective for addressing areas of the body that have reached a plateau in their healing progress such as joint pain, chronic pain, or even hair loss.
Conditions PRP Injections Can Treat:
- Achilles Tendonitis & Tears
- Ankle Sprains & Instability
- Arthritis – Degenerative Joint Disease
- Cartilage Defects
- Degenerative Disc Disease
- Foot Pain
- Golfers Elbow
- Hip Pain – Arthritis, Tendonitis
- Knee Pain – Arthritis, Tendonitis
- Ligament Injuries
- Neck Pain
- Osteoarthritis – All Joints
- Patellar Tendonitis
- Pes Anserine Bursitis
- Plantar Fasciitis
- Rotator Cuff Tears/Tendonitis
- Tendinosis
- Runners Knee
- Sacroiliac Joint Pain
- Shoulder Pain-Arthritis/Tendon
- Spinal Arthritis
- Sports Injuries
- Tarsal Tunnel Syndrome
- Tendonitis
- Tennis Elbow
- Trochanteric Bursitis
- Whiplash – Chronic pain
What Do PRP Injections Do?
Physicians employing PRP therapy to address osteoarthritis hypothesize that platelet-rich plasma may have the following effects:
- Inhibit inflammation and decelerate the progression of osteoarthritis.
- Enhance the generation of natural lubricating fluid within the joints, thereby alleviating painful joint friction.
- Contain proteins that modify a patient’s pain receptors, diminishing the sensation of pain.
- Enhance joint function by expanding the joint’s range of motion and reducing extended stiffness.
PRP formulations can exhibit variability because they originate from the blood of individual patients, and each person’s blood possesses unique characteristics. Additionally, various physicians may adopt diverse methodologies when formulating and preparing PRP solutions for injection.
How is Platelet-rich Plasma Made?
The typical method for creating PRP involves subjecting a blood sample from the patient to centrifugation. This involves placing a vial of blood into a high-speed centrifuge. During this spinning process, the blood separates into distinct layers:
- Red blood cells, constituting around 45% of the blood, are compelled to settle at the bottom of the vial.
- The white blood cells and platelets together form a thin intermediary layer known as the buffy coat, comprising less than 1% of the centrifuged blood.
- The uppermost layer consists of “platelet-poor” plasma, which has a low concentration of platelets and makes up roughly 55% of the centrifuged blood sample.
Subsequent to completing the centrifugation process, the medical practitioner or technician will extract the vial from the centrifuge and prepare the PRP solution for injection.
The centrifugation speed and duration can vary, influencing the composition of the PRP produced. Currently, there is no unanimous agreement regarding the centrifugation process that yields the most favorable outcomes for osteoarthritis treatment.
What are Platelets?
Much like red and white blood cells, platelets are a natural constituent of blood. Platelets, in isolation, do not possess inherent regenerative or curative attributes. Instead, they release growth factors and various proteins that oversee cell division, trigger tissue rejuvenation, and facilitate the healing process. Platelets also play a crucial role in blood clotting, as individuals with malfunctioning or insufficient platelets tend to experience excessive bleeding from wounds.
What are in PRP Injections?
PRP injections are not identical across the board. The precise composition of platelet-rich plasma varies based on multiple factors, including the platelet concentration, the white blood cell concentration, and the inclusion of additives.
Concentration of Platelets
Typical blood contains 150,000 to 450,000 platelets per microliter (μL), and the platelet concentration in platelet-rich plasma can range from 2.5 to 9 times this amount. The actual concentration varies based on factors like the individual’s blood characteristics, the volume of blood collected, the centrifugation process (e.g., speed and duration of rotation), and other clinical preparation techniques.
While it might appear logical that plasma with the highest possible platelet concentration would yield superior results compared to plasma with lower concentrations, this is not necessarily the case. According to one laboratory study, plasma with concentrations 2.5 times that of regular blood was deemed optimal, and higher concentrations might actually impede new cell growth.
White Blood Cell Count
The immune system relies on white blood cells to combat infections, leading experts to speculate that white blood cells may impede the healing process of tissues. This interference can subsequently foster inflammation, the formation of scar tissue, and harm to neighboring tissues.
Similar to platelet concentration, the concentration of white blood cells is influenced by clinical preparation techniques and the characteristics of an individual’s blood.
Additives
In some cases, specific substances can be introduced into the PRP. These substances, known as thrombin and calcium chloride, serve to artificially trigger the activation of platelets. This activation leads to platelet clotting and the release of platelet growth factors. Some researchers propose that these additives may potentially augment the regenerative capabilities of platelet-rich plasma.
It’s worth noting that collagen present within tendons and the thrombin released due to the injection process itself may trigger platelet activation, even without the use of additional additives. The precise impact of these factors on the effectiveness of PRP therapy remains not fully understood.
Platelet-Rich Plasma Injection Procedure Studies
Researchers investigating PRP injections and its application in treating osteoarthritis typically focus on patients dealing with knee osteoarthritis, a condition projected to impact nearly half of the U.S. population at some point in their lives. Below are descriptions of two clinical studies concerning the use of PRP for knee arthritis:
Study 1 Published in 2013, this study involved 78 patients afflicted with osteoarthritis in both knees, totaling 156 knees. Each knee received one of three treatments: either one PRP injection, two PRP injections, or one placebo saline injection. Researchers assessed the patients’ knees at the 6-week, 3-month, and 6-month marks post-injection. The findings revealed the following:
- Knees treated with one or two PRP injections experienced decreased pain and stiffness, along with improved knee function at the 6-week and 3-month evaluations.
- By the 6-month mark, the positive effects had somewhat diminished, though pain and function were still better compared to before the PRP treatment.
- The group that received placebo injections saw a minor increase in pain and stiffness, alongside a decline in knee function.
- The platelet-rich plasma used in this study had three times the platelet concentration of regular blood and had been filtered to eliminate white blood cells.
Study 2 Furthermore, a smaller study examined patients with mild knee pain, which had persisted for an average of 14 months. Each arthritic knee underwent an MRI to assess joint damage and subsequently received a single PRP injection. Evaluations of the patients’ knees were conducted at the 1-week, 3-month, 6-month, and 1-year intervals. Additionally, each knee underwent a second MRI after one year. The research revealed the following:
- One year after receiving the PRP injection, most patients experienced less pain compared to the previous year, although the pain had not necessarily vanished.
- MRI results indicated that the degenerative process did not advance in the majority of knees.
- While knee cartilage did not appear to regenerate in patients, the fact that arthritis did not worsen could hold significance. Existing evidence suggests an average annual loss of 4 to 6% of cartilage in arthritic joints.
PRP injections are typically performed as outpatient procedures. Since the patient’s blood needs to be drawn and prepared for injection, the procedure usually takes anywhere from 45 to 90 minutes.
Knee Injection
The decision regarding whether a patient receives a one-time injection or a series of injections spaced over weeks or months depends on the patient’s preferences and the doctor’s recommendations. In the case of a series of injections, a doctor may propose drawing a single blood sample during the initial visit and utilizing fresh PRP for the first injection. The remaining PRP can then be frozen and thawed as necessary for subsequent injections. Nevertheless, some experts have reservations about the impact of freezing and thawing on PRP’s efficacy and, therefore, advocate for a separate blood draw for all PRP injections. At Opdahl Regenerative Medicine, we opt for the approach of conducting a distinct blood draw before each PRP injection. This choice aims to ensure the best possible outcomes, particularly for patients dealing with severe arthritis who require a series of injections.
Pre-Injection Precautions
The American Academy of Orthopedic Surgeons provides the following pre-injection recommendations for patients:
- Refrain from corticosteroid medications for 2 to 3 weeks before the procedure.
- Discontinue the use of non-steroidal anti-inflammatory drugs (NSAIDs), like aspirin or ibuprofen, as well as arthritis medications such as Celebrex, a week prior to the procedure.
- Avoid anticoagulation medication for 5 days leading up to the procedure.
- Ensure adequate hydration by consuming ample fluids on the day before the procedure.
- In some cases, patients may necessitate anti-anxiety medication immediately prior to the procedure.
After the PRP Injection: Immediate Follow-up Care
According to the American academy of Orthopaedic Surgeons patients are recommended to rest and refrain from exerting excessive pressure on the impacted joint after any PRP injections.
Physicians may prescribe or advise patients to:
- Avoid anti-inflammatory pain medication, as an alternative pain medication may be provided by the doctor.
- Utilize a brace or sling to safeguard and immobilize the affected joint; patients receiving injections in the ankle, knee, or hip might be encouraged to use crutches.
- Apply a cold compress multiple times daily, with each session lasting 10 to 20 minutes, to help reduce post-injection discomfort and swelling.
Does Insurance Cover PRP Injections?
Regrettably, non-surgical PRP injections are typically not reimbursed by insurance plans or providers due to their classification as “experimental” treatments, primarily due to a perceived lack of FDA-specific procedure evidence. It’s important to note that “experimental” therapies are typically conducted within clinical trials, which is not the case here; we offer FDA-cleared PRP Therapy to eligible patients following a comprehensive medical evaluation. However, this treatment is not universally available.
What Does This Imply for You? While certain insurance companies might cover the initial consultation or examination fees, they usually won’t cover PRP costs in most clinics. Fortunately, at Opdahl Regenerative Medicine, our patients can explore financing options to assist with the expenses of most procedures.
How Much Do PRP Injections Cost?
The cost of each PRP session will significantly hinge on the following factors:
- The number of therapy sessions required.
- The severity and extent of your medical condition.
- The duration you’ve been dealing with the issue.
- The number of areas targeted for improvement.
Side Effects of PRP Injections
PRP therapy offers a valuable alternative to surgeries for back, shoulder, knee, and other medical conditions, eliminating the need for extended recovery periods, incision-related discomfort, and other surgical complications. In fact, when patients undergo their prescribed PRP injection regimen, they experience virtually no downtime, allergic reactions, or rejection issues since the PRP is derived from their own body.
Patients can conveniently receive these injections in their doctor’s office and resume their regular activities afterward. Nevertheless, a few individuals may encounter minor side effects, which can include:
- Slight bleeding.
- Possible infection.
- Discomfort at the injection site (usually alleviated through the application of anesthetic before PRP injection).
- Mild swelling, redness, and temporary skin discoloration, which typically resolve swiftly.
Learn More About Alternative Ways to Alleviate Your Pain
Get back to doing the things you love, faster & without surgery.
Request an Appointment Today!
References:
Center for Disease Control. Spotlight Osteoarthritis: Lifetime Risk of Symptomatic Knee Osteoarthritis. Updated October 20, 2010. www.cdc.gov. Accessed October 22, 2013.
Patel S, Dhillon MS, Aggarwal S, Marwaha N, Jain A. Treatment with platelet-rich plasma is more effective than placebo for knee osteoarthritis: a prospective, double-blind, randomized trial. Am J Sports Med. 2013 Feb;41(2):356-64. doi: 10.1177/0363546512471299. Epub 2013 Jan 8. PubMed PMID: 23299850.
Halpern B, Chaudhury S, Rodeo SA, Hayter C, Bogner E, Potter HG, Nguyen J. Clinical and MRI outcomes after platelet-rich plasma treatment for knee osteoarthritis. Clin J Sport Med. 2013 May;23(3):238-9. doi: 10.1097/JSM.0b013e31827c3846. PubMed PMID: 23238250.
Eckstein F, Cicuttini F, Raynauld JP, et al. Magnetic resonance imaging (MRI) of articular cartilage in knee osteoarthritis (OA): morphological assessment. Osteoarthr Cartilage. 2006;14:46–75.
Raynauld JP, Martel-Pelletier J, Berthiaume MJ, et al. Long term eval- uation of disease progression through the quantitative magnetic reso- nance imaging of symptomatic knee osteoarthritis patients: correlation with clinical symptoms and radiographic changes. Arthitis Res Ther. 2006;8:21.
Lee KS, Wilson JJ, Rabago DP, Baer GS, Jacobson JA, Borrero CG. Musculoskeletal applications of platelet-rich plasma: fad or future? AJR Am J Roentgenol. 2011 Mar;196(3):628-36. doi: 10.2214/AJR.10.5975. Review. PubMed PMID: 21343507.
Kolata G. As Sports Medicine Surges, Hope and Hype Outpace Proven Treatments. The New York Times. Sept 4 2011. www.nytimes.com. Accessed October 8, 2013.